ADV- Lesson 3- Ventilation During CPR
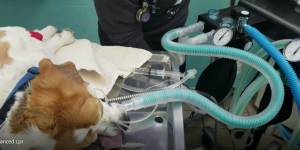
Ventilation is more effective with a cuffed endotracheal tube than via mouth-to-snout ventilation. Chest compressions should not be stopped to facilitate intubation. Staff should be trained to intubate a patient in lateral recumbency. It is recommended that you practice this frequently when intubating patients for elective anesthetic procedures. Primary respiratory arrest is more common in dogs and cats than in people. Since stroke volume in CPR only delivers 30% of normal volume, diverting blood to the periphery results in decreased perfusion to the core organs, such as the brain, heart, and lungs. Increased intracranial pressure can result from cerebral vasodilation. In intubated patients, ventilation should be done at 10 breaths per minute, 1 breath every 6 seconds. This lower respiration rate helps avoid hyperventilation. Less CO2 is delivered to the lungs during CPR because the cardiac output is lower.
The main goals of respiratory support in CPR is to ventilate the animal and increase excreted carbon dioxide produced by the tissues and provide oxygenation which transports oxygen into the blood. There are two types of pressure breaths: spontaneous and positive pressure breaths.
Spontaneous Breaths– This is when negative pressure in the chest draws air into the respiratory system on inhale. This happens during natural breathing.
Positive Pressure Breaths– This is when air is forced into the airway such as in CPR. Serious side effects of CPR can happen if the rescuer uses incorrect ventilation techniques.
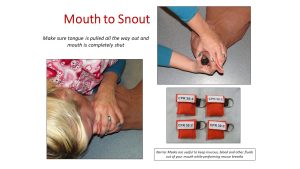
Mouth to Snout Resuscitation
This is accomplished by pulling out the animal’s tongue, closing the mouth, and placing your mouth around both nostrils securely. Blow into the animal’s airway watching for the chest to expand. When you feel resistance as the lungs are inflated, take your mouth off the nostrils and the lungs will deflate. It is ideal to stop compressions before breathing into the animal’s airway. The reason for this is that air will flow into the esophagus and stomach rather than into the lungs when the lungs are compressed during chest compressions. [4]
